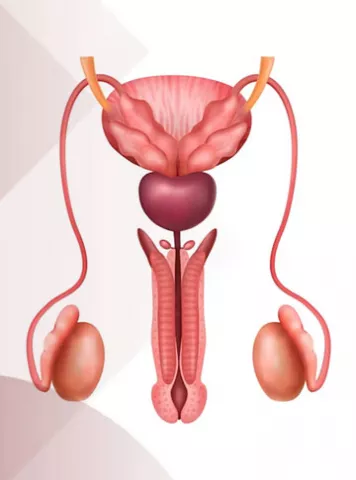
What are the best ways to increase sperm count?
Let's understand how to increase sperm count by food, exercise, medicines, lifestyle changes and know all the important aspects and methods of how to improve sperm count & motility in this article.
What is a low sperm count?
Recent studies have revealed that the average sperm count has been falling worldwide in the male population. This revelation in the fertility health of the males is concerning and calls for immediate medical advice to be followed. Therefore, several approaches on how to increase sperm motility, sperm count, and overall health can be resorted to.
Male infertility is often the result of a low sperm count. The World Health Organization defines low sperm count as having less than 15 million sperm per millilitre of sperm or fewer than 39 million sperm per ejaculate. As a general guideline, if you haven't conceived after a year of regular unprotected sexual intercourse, you should consult a trustworthy doctor regarding how to make sperm stronger for pregnancy.
There are several factors that might contribute to male infertility, including genetics, general health, physical fitness, illnesses, age, and environmental toxins. Fertility declines with age due to the loss of normal sperm and the capacity of sperm to migrate, especially beyond the age of 50. Yet, several dietary and lifestyle changes, as well as natural treatments, can support the hormones that regulate sperm production, which may assist in promoting healthy sperm growth and increasing sperm count.
What works best to increase sperm count?
Here are some best methods on how to increase sperm volume.
-
Get Enough Rest and Do Regular Exercise
Regular exercise can increase testosterone levels and enhance fertility in addition to being beneficial for overall health. Research revealed that active males had greater testosterone levels and superior sperm quality compared to sedentary ones. Although excessive exercise may have the opposite impact and perhaps lower testosterone levels, it should be avoided. Making physical activity a priority should be your first concern if you are thinking about how to increase sperm count naturally.
-
Take D-Aspartic Acid Supplements
D-aspartic acid (D-AA), which is sold as a dietary supplement, is one form in which aspartic acid is present. Semen, sperm, and a few glands, notably the testicles, contain the majority of the body's D-AA supply. Researchers believe that D-AA affects male fertility. In fact, compared to males who are fertile, infertile men have much lower D-AA levels. Studies indicating that D-AA supplementation may raise levels of testosterone, the male sex hormone that is crucial for male fertility, corroborate this. Using 3 grams of D-AA tablets daily for two weeks raised testosterone levels in healthy males by 42%, according to another controlled research. But it is advisable to consult with your doctor first.
-
Avoid using medicines which can affect fertility
Certain pharmaceutical medications may reduce the production of healthy sperm. But, as soon as the male quits using the drug, his sperm count ought to revert to normal or even rise. Medicines that might momentarily reduce sperm development and production include:
- Antibiotics
- Anti-inflammatories
- Anti-androgens
- Antipsychotics
- Antidepressants
- Exogenous or supplementary testosterone
- Anabolic steroids may still have an impact on sperm count a year after discontinuing the medication
If men suspect that a medicine, they are presently taking may be lowering their sperm count or impacting their fertility, they should visit a healthcare professional immediately.
-
Get enough Vitamin C
Several studies suggest that taking antioxidant supplements like Vitamin C might boost fertility. Oxidative stress develops when the body's reactive oxygen species (ROS) levels reach harmful levels. It happens when sickness, age, unhealthy lifestyle, or environmental contaminants overwhelm the body's natural antioxidant defences. Antioxidants, particularly Vitamin C, should be consumed in sufficient amounts to help mitigate some of these negative effects. Several research studies suggest that supplemental vitamin C may improve the quality of semen. Moreover, supplementing with vitamin C led to an increase in sperm count and motility while significantly reducing the number of sperm cells with defects.
-
Consume More Vitamin D
An increase in blood levels of vitamin D was linked to better male fertility, according to medical research. The sperm count may also be negatively impacted by a calcium deficit. Vitamin D might be important for both male and female reproduction. This extra vitamin may help to increase testosterone levels. When they consumed 3,000 IU of vitamin D3 every day for a year, their testosterone levels rose by around 25%.
-
Get Enough Zinc & Folate
Several studies indicate that ingesting folate and zinc together may enhance the general health of sperm, including concentration and count. Animal products, including meat, fish, eggs, and shellfish, are rich sources of zinc, a vital element. Observational studies have demonstrated a link between low testosterone levels, poor sperm quality, a higher risk of male infertility and low zinc status or deficiency. In addition, persons with low zinc levels who take zinc supplements had higher testosterone and sperm counts.
-
Consider Taking Ashwagandha
Ashwagandha, often known as Indian ginseng, has long been used in traditional medicine as a treatment for several types of sexual dysfunction. According to studies, ashwagandha may increase testosterone levels, therefore enhancing male fertility. One study found that consuming 675 mg of ashwagandha root extract daily for three months substantially increased fertility in males with low sperm cell counts. In particular, it raised sperm counts by 167%, semen volume by 53%, and sperm motility by 57% compared to starting points in the trial.
-
Consume Fenugreek Supplements
Fenugreek has long been used as a home cure for unhealthy sperm, and experts believe it may increase sperm count. One researcher evaluated the results of ingesting 500 mg of fenugreek extract daily in 30 males who exercised four times per week. In fact, a 2017 study discovered that the patented substance Furosap, which producers created from fenugreek seeds, dramatically increased sperm count and overall sperm quality.
-
Relax & Relieve Your Stress
Stress can impact both your fertility and your level of sexual satisfaction. Researchers believe that the cortisol hormone may contribute to some of these detrimental effects of stress. Stress for a long period of time raises cortisol levels, which negatively affects testosterone in a substantial way. Typically, when cortisol levels increase, testosterone levels decrease. Going for a walk outdoors, practising meditation, doing some exercise, or hanging out with friends may all help you manage your stress and can be the answer to how to make sperm thicker and stronger.
Most men experience infertility at some point in their lives. If you and your spouse are having trouble getting pregnant, you can always contact the fertility expert at Indira IVF to know the root cause and get the right treatment.
Book a Free Consultation with our IVF Doctors today!
Articles
2023

Male Infertility Guide to infertility treatments
अशुक्राणुता (एजुस्पर्मिया) के कारण, लक्षण और उपचार (Azoospermia in Hindi)
माता-पिता बनने से महरूम रहना भ...
2023


What is abnormalities in sperm?
Sperm is a crucial component of the reproductive system in males. It is a spec...
2023


Female Infertility Male Infertility
How many days Sperm Live in Female Body after Intercourse?
While it depends on the correct circumstances and the stage of the woman's men...
2023


Male Infertility Infertility Tips
Hyperspermia: Causes, Symptoms, Diagnosis & Treatment
What is Hyperspermia? Hyperspermia is a condition where an individual produ...
2022

पुरूष निःसंतानता का एक कारण वेरिकोसिल आधुनिक तकनीकों से संभव है पिता बनना
पुरूष निःसंतानता शब्द कुछ सा�...
2023
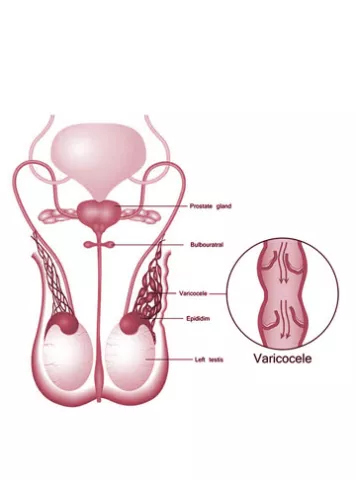

Male Infertility Guide to infertility treatments
What is Varicocele? Varicocele is a medical condition where the veins in th...
2022


Infertility Tips Male Infertility
Male Infertility Medicine: How does IVF help Male Infertility
What is Male Infertility? Male infertility is the lack of ability to genera...
2022

Infertility Tips Male Infertility
In addition to spermatozoa, semen is composed of prostatic and seminal vesicul...
2022


Infertility Tips Male Infertility
Foods for Increasing Sperm Count A healthy diet is the ultimate solution to...
Pregnancy Calculator Tools for Confident and Stress-Free Pregnancy Planning
Get quick understanding of your fertility cycle and accordingly make a schedule to track it