Infertility is inability to conceive naturally. It can affect the very young age group also as fertility in them is taken for granted. Ultrasonography has upsurged as an important diagnostic as well as therapeutic tool which not only guides the appropriate and timely treatment but also has improved the quality of care in women who are going for advance treatment options like in vitro fertilization.
Imaging with a transvaginal ultrasound is a simple, safe, efficient and a non-invasive method to evaluate fertility potential of a female.
INFERTILITY ULTRASOUND SCAN BASICS
Ultrasound scans work by using high-frequency sound waves to create an image of female internal organs. Transvaginal transducer is used to evaluate the female genital tract anatomy.
The women needs to empty her bladder ; pass urine for a better evaluation.
Timing of evaluation
Timing of the scan is also important to maximize the quality of information and depends on the doctor as what exactly is suspected. It can be done either in early cycle which is the follicular phase or mid cycle (ovulatory phase) or secretory phase (post ovulatory) of a regular (28 day) menstrual cycle.
The antral follicle count can be judged on day 2/3 of a cycle. Serial scans during early proliferative phase can tell us both about the follicular growth and endometrial pathology. Post ovulatory scan can reveal a corpus luteum ( ovulation has occurred) and the ability to assess the endometrial response to follicular development
DIAGNOSTIC USE OF ULTRASONOGRAPHY IN INFERTILITY INVESTIGATIONS: THE OVARY
Assessment of ovarian follicular development
The dominant follicle(fig 1) continues to grow at a rate of about 2 mm per day and reaches ~18–20 mm before rupture (ovulation). This Follicle growth can be assessed on serial ultrasounds and follicular monitoring gives a good idea about appropriate growth of dominant follicle and timely ovulation .The optimal time to schedule intercourse or perform an intrauterine insemination (IUI) in spontaneous and stimulated cycles can thereby be estimated.
OVARIAN PATHOLOGIES
POLYCYSTIC OVARY
Polycystic ovaries (PCO) are described on ultrasound scan as the presence of 12 or more follicles in each ovary measuring 2-9 mm in diameter, and/or increased ovarian volume (>10 ml)1 (fig2). Patients with PCO may require ovarian stimulation and are more likely to develop Ovarian Hyperstimulation Syndrome (OHSS).
Endometriomas
These are fluid-filled cysts that typically contain a “chocolate” colored fluid that is presumed to arise from sequestered menstrual effluent. Fertility potential is impaired when endometriosis distorts the normal tubo-ovarian relationship. A ‘typical’ endometrioma is a unilocular cyst with a regular wall and appears as ‘ground glass’ on TVS(fig 3).
Transvaginal scan can also diagnose luteal cysts, cystadenomas, pyosalpinx, dermoids and ovarian cancers, because, in these masses, the cyst content (blood, mucus or pus) may display low-level echoes on ultrasound. Moreover, power Doppler can be of help in differentiating different types of cysts.. Endometriotic cysts are associated with scanty vascularization of the cyst wall, while non-endometriotic cysts, particularly luteal cysts and ovarian cancers, are characterized by rich vascularization of the wall and the presence of arterial flow within the echogenic areas of the cyst.
THE OVIDUCT
Normal FALLOPIAN tube is usually invisible on ultrasound.
Hydrosalpinx is diagnosed as well-constrained fluid accumulation in the adnexa.
THE UTERUS
Uterine anatomy: The uterine body is comprised of serosa, myometrium and intracavitary glandular epithelium called endometrium. The endometrium respond to the reproductively active hormones and hence, the phase of the menstrual cycle can be estimated by examining endometrial patterns with ultrasonography .During the follicular phase, estrogen results in a progressive increase in endometrial thickness (triple stripe echotextural pattern).Following ovulation, growth and branching of the endometrial glands due to progesterone makes endometrium hyperechoic and homogeneous.
MEASURING THE ENDOMETRIUM
An important aspect of the fertility scan is the examination of the endometrium. A trilaminar appearance(fig4) with a minimum thickness of 7mm and a uterine artery pulsatility index of less than 3 are regarded as reliable markers of good endometrial receptivity.
Uterine polyps
These are growths that occur in the endometrium. Endometrial polyps may be visualized at transvaginal ultrasound as non-specific endometrial thickening, they may also be identified as focal “pearl-shaped” masses within the endometrial canal. These polyps can interfere with implantation, effectively preventing an embryo from attaching to the uterine wall.
Endometrial synechiae
Synechiae or adhesions, may form between areas where destruction of basal endometrium has occurred. They may extend across the uterine cavity and may obliterate or obstruct the cavity. Endometrial damage may be suspected when portions of, or the entire, endometrial surface remains thin and irregular in contour and hyperechoic throughout the cycle rather than changing patterns in association with the reproductively active hormones.
THREE-DIMENSIONAL IMAGING OF THE ENDOMETRIUM
Three-dimensional (3D) ultrasound enables capture of a volume of uterine cavity that can be reconstructed and displayed in any plane( fig 5). This advance now makes it possible to examine the uterus in a coronal orientation, so MRI is no longer required to assess uterine shape . Three-dimensional ultrasound evaluation of the uterus is useful before ART for assessing congenital uterine anomalies. The ability of an individual to conceive is not prevented merely by the presence of a uterine anomaly, but these are also involved in first trimester pregnancy loss.
SALINE INFUSION SONOHYSTEROGRAPHY
It is a procedure to evaluate the shape of the uterine cavity. The ultrasound examination is continued while sterile saline is put intside the uterine cavity. The saline solution fills the uterus, helping to outline the uterine walls and cavity. This shows abnormalities such as fibroids, polyps, or scar tissue inside the uterus.
MYOMETRIUM
Many important gross abnormalities of the uterus such as congenital anomalies (septate uterus, bicornuate and didelphys uterus), large fibroids and adenomyomas can be easily diagnosed. Large fibroids that grossly distort the endometrial cavity require removal before fertility treatment begins.
Adenomyosis is diagnosed when endometrial glands and stroma (salt and pepper appearance) are found in uterine myometrium. Color flow mapping of the myometrium with transvaginal ultrasonography has been used to evaluate adenomyosis.
THERAPEUTIC USES OF ULTRASONOGRAPHY IN INFERTILITY
MONITORING THE COURSE OF OVARIAN STIMULATION
Ovarian stimulation is now routinely performed to provide numerous oocytes for IVF and ICSI therapies. Ultrasonography is required to monitor changes in multiple growing follicles during FSH therapy.
OOCYTE RETRIEVAL
Ultrasound-guided oocyte retrieval is now a routine in IVF. Oocyte retrieval is most often completed in a clinic setting using short-acting intravenous analgesia .An aspiration needle is introduced via the guide, inserted through the vaginal fornix, and directed to the ovaries so that many ovarian follicles can be sequentially aspirated without reinsertion of the needle.
Conclusion
Ultrasonography has allowed us to understand folliculogenesis, ovulation, luteal function, uterine response, conception, and implantation, and to apply this knowledge to explain and explore normal reproduction and infertility. As the technology of ultrasonography continues to evolve, we anticipate this indispensable tool will continue to shape our knowledge and enhance our ability to care for women.
Articles
2023

Guide to infertility treatments IVF
एक्टोपिक प्रेगनेंसी के लक्षण, कारण और इलाज
प्रेगनेंसी की खबर महिला को का�...
2023


Guide to infertility treatments
Hypertension- How it impacts Fertility and Pregnancy
Blood pressure problems are no longer just an old-age problem. It is steadily ...
2023

Male Infertility Guide to infertility treatments
अशुक्राणुता (एजुस्पर्मिया) के कारण, लक्षण और उपचार (Azoospermia in Hindi)
माता-पिता बनने से महरूम रहना भ...
2023


IVF Guide to infertility treatments
टेस्ट ट्यूब बेबी का खर्च कितना आता है (What is the test tube baby cost in hindi)
पिछले कुछ वर्षों में टेस्ट ट्�...


Guide to infertility treatments Infertility Tips
पीआईडी: पेल्विक इनफ्लैमेटरी डिजीज और निःसंतानता
पीआईडी - पेल्विक इनफ्लैमेटरी �...
2022

Guide to infertility treatments IVF
थाइरायड असंतुलन के कारण हो सकती है निःसंतानता, आईवीएफ से कैसे हो सकता है।
पिछले कुछ वर्षों में थायराइड �...


IVF Guide to infertility treatments
भारत में आईवीएफ ट्रीटमेंट में कितना खर्चा होता है
पिछले कुछ वर्षों में टेस्ट ट्�...
2023
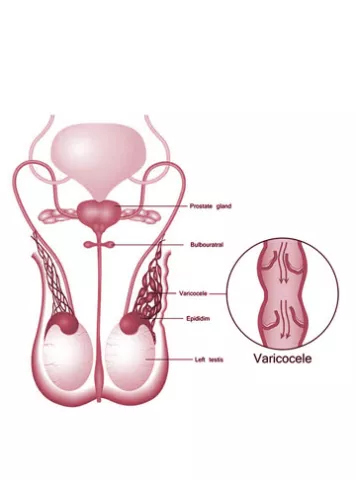

Male Infertility Guide to infertility treatments
What is Varicocele? Varicocele is a medical condition where the veins in th...
2022

Guide to infertility treatments
Infertility is inability to conceive within one year of unprotected intercours...
Pregnancy Calculator Tools for Confident and Stress-Free Pregnancy Planning
Get quick understanding of your fertility cycle and accordingly make a schedule to track it